What is the story of wearing face masks during exercise and in particular the physiological effects upon breathing?
During Covid millions of people have been wearing masks and arguing about masks but what about physiological effects? You will know that for years some athletes tried “altitude masks” with mixed results. Basically, they do make breathing more difficult (that was the point….a harder stimulus), but the effect is short-lived and adaptation hard to show. But what this does demonstrate, is that any kind of effective face mask is altering the physiology of breathing (eg tidal volume) and perception of breathing (ie “its harder”) and possibly respiratory gas exchange (see below). But let’s start with the most basic question, what is the effect on performance (whilst wearing a mask)……
Performance with vs without Masks
Let’s take a few examples. Egger (2021) randomized 16 well-trained athletes to do cycling erg tests to exhaustion without mask (NM), with surgical mask (SM) and FFP2 mask (FFP2). There was a large effect (-6%) of masks on performance with a significant reduction of maximum performance as follows
No mask =377w ± 40
Surgical mask (SM)= 355w ± 41
FFP2 mark = 364w ± 43
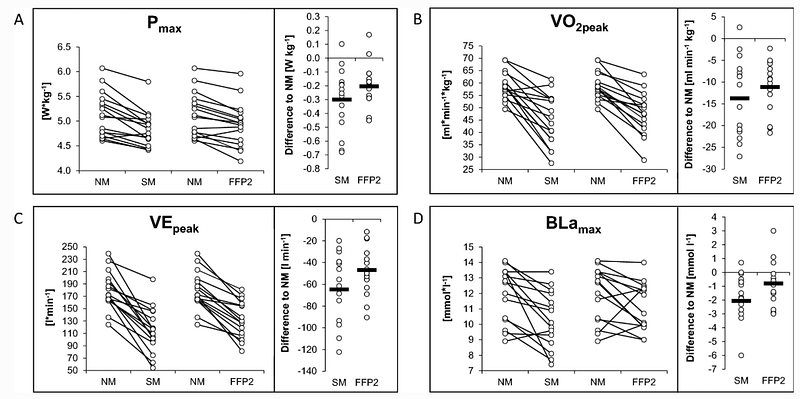
A maximum performance (Pmax). B peak oxygen consumption (VO2peak). C peak minute ventilation (VEpeak), D maximum blood lactate concentration (BLamax). W Watt
Most (11 of 16) subjects reported acute shortness of breath (dyspnea) from the suction of the wet and deformed mask!
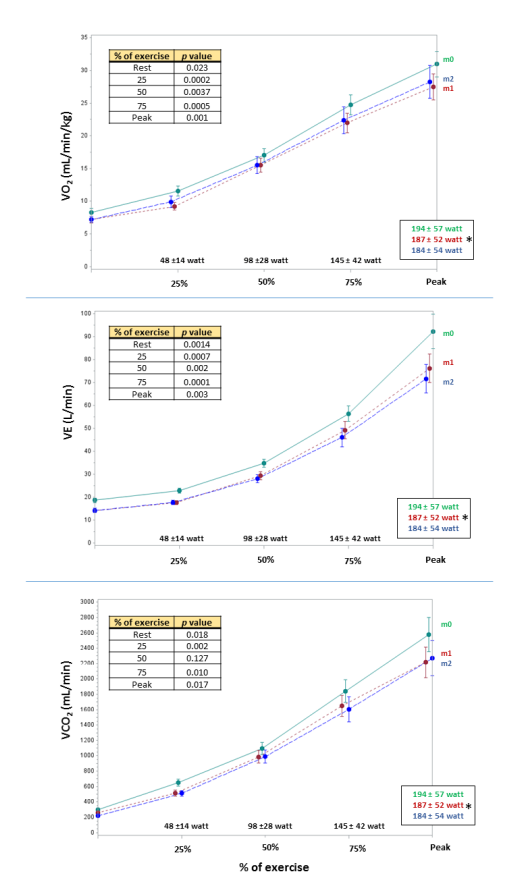
Mapelli 2021 (ref) charted the difference in 12 healthy subjects who did three cardiopulmonary exercise tests with and without surgical and with FFP2 mask. Using spirometry, from no mask to surgical to FFP2, a progressive reduction of Forced expiratory volume in 1 second and Forced vital capacity was observed Rest ventilation, O2 uptake (V̇O2) and CO2 production (VCO2) were progressively lower with a reduction of respiratory rate. but there was no significant difference in oxygen saturation.
What about in runners? Driver et al (ref) randomised 31 healthy adults aged 18–29 years to treadmill running with and without a cloth face mask. Wearing a cloth face mask led to a significant reduction in exercise time, maximal oxygen consumption (VO2max) (−818±552 mL/min, p<0.001), minute ventilation (−45.2±20.3 L/min), maximal heart rate (−8.4±17.0 beats per minute, p<0.01) and increased dyspnoea (1.7±2.9, p<0.001).
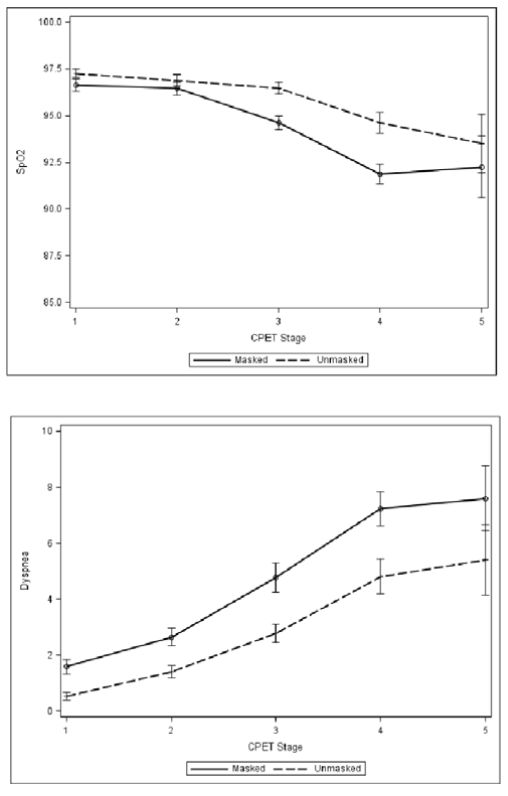
Cloth face masks led to a 14% reduction in exercise time and 29% decrease in VO2max. Compared with no mask, participants reported feeling increasingly short of breath and claustrophobic at higher exercise intensities while wearing a cloth face mask.
Here is a quick summary of performance studies (from the driver paper)
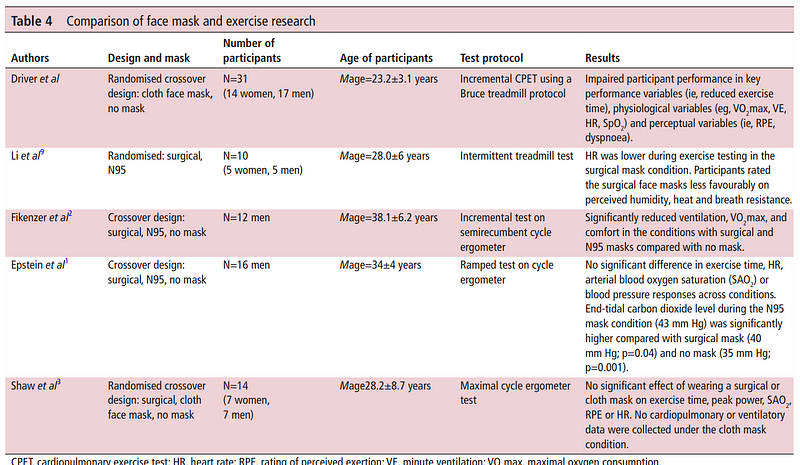
How Much Harder does it feel?
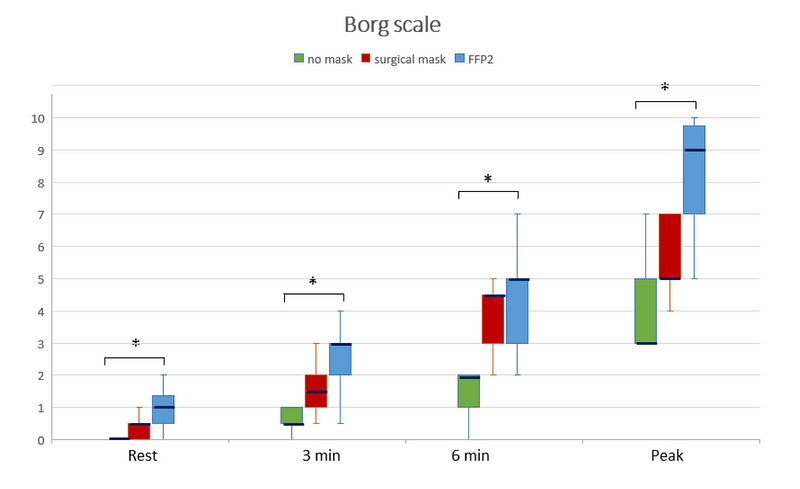
The above study by Mapelli 2021 (ref) charted the difference in 12 healthy subjects who did three cardiopulmonary exercise tests with and without surgical and with FFP2 mask. 3mins exercise with a simple surgical mask was equivalent in effort to 6min with no mask!
Is there an effect on gas exchange in athletes?
Porcari studied 12 athletes and found mask wearers showed significantly lower oxygen saturation values (SpO2%) during exercise (SpO2 of 94% for mask wearers versus 96% for mask-less, p < 0.05) [ref], which can be explained by an increased dead space volume and increased resistance during breathing. The measured oxygen saturation values were significantly lower than the normal values in the group of mask wearers, which indicates a clinical relevance.
Jagim examined weightlifters (ref). Twenty male recreational weight lifters completed 2 training sessions of back squat and bench press (6 sets of 10 repetitions at 85% of 5-repetition maximum and seventh set to failure) as well as a maximal effort sprint test (18% body mass) with the mask (ETM) and without the mask (NM). There was a significant decrease in oxygen saturation SpO2 when performing back squats in the mask group after only 1 min of exercise compared to the mask-free group (p < 0.001)
Pifarré studied eight middle-aged subjects (19–66) doing push ups, the gas content for O2 and CO2 under the masks was determined before and after exercise. Even at rest, the oxygen availability under the masks was 13% lower than without the masks and the carbon dioxide (CO2) concentration was 30 times higher. Under stress (Ruffier test), the oxygen concentration (% O2) below the mask dropped significantly by a further 3.7%, while the carbon dioxide concentration (% CO2) increased significantly by a further 20% (statistically significant with p < 0.001) [ref].
Conclusions
Yes it’s true, simple cloth masks are pretty “leaky” to gas exchange meaning overall effects will be small (but that’s also one reason why they don’t really work against air-borne viruses!). However for decades athletes have used masks to intentionally restrict breathing efficiency and train with a harder stimulus. N95 masks leads to a mean increment of 25% inspiratory and expiratory flow resistances. Breathing harder to some extent compensates for slight changes in CO2 which regulates pH in the CSF. A 10mmHg rise in co2 stimulates ventilation around 0.5L/min.
So raw changes in gas exchange are compensated tightly by respiratory drive (ie effort) and dysregulation effects are “small”. However even “small” effect on inhaled oxygen or expired CO2 can be significant in terms of discomfort. Studies show that there is a measurable increase in expired co2 (“end-tidal carbon dioxide”) around 5–8mmHg (or 20%) with masks which is due to re-breathing of the expired air causing mild hypercapnia (o2 is normally maintained ok).
Several studies dismiss mild hypercapnia (good review here: https://www.mdpi.com/1660-4601/18/8/4344/htm?s=09), but the above functional / performance studies show a definite effect. And remember it is co2 that is the main breathing stimulus not o2.
Finally this study from Epstein 2020 puts numbers on expired co2 with exercise….
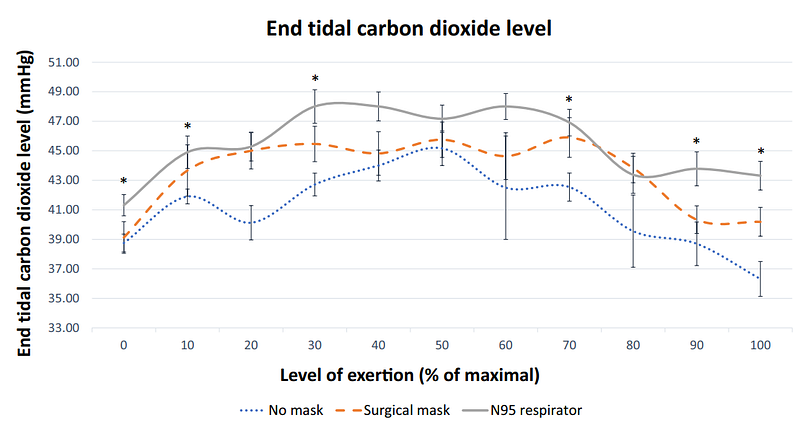
Bottom line is:
Exercising with a surgical mask or a N95 mask feels harder, slows you down and very likely gives a small but significant increase in carbon dioxide.
This effect will be larger in more vulnerable people and with harder exercise.
There is a theoretic training benefit from “altitude mask simulation” but it almost impossible to maintain the conditions long enough and consistently enough to get a adaptation benefit
There is also an implication for wearing masks even when not exercising, as poor gas exchange in dead space is a worry that almost no one is talking about.
