If you follow “healthy diets” in the news as closely as me then you will likely be very confused by now…..almost every diet and every nutrient has been hailed as both helpful and harmful!

In order to get an answer, I think it’s best to concentrate on actual studies, ideally involving a randomized design and ideally with solid outcomes such as mortality (survival). We will also focus on human studies, if you want to see animal studies then here is a summary:
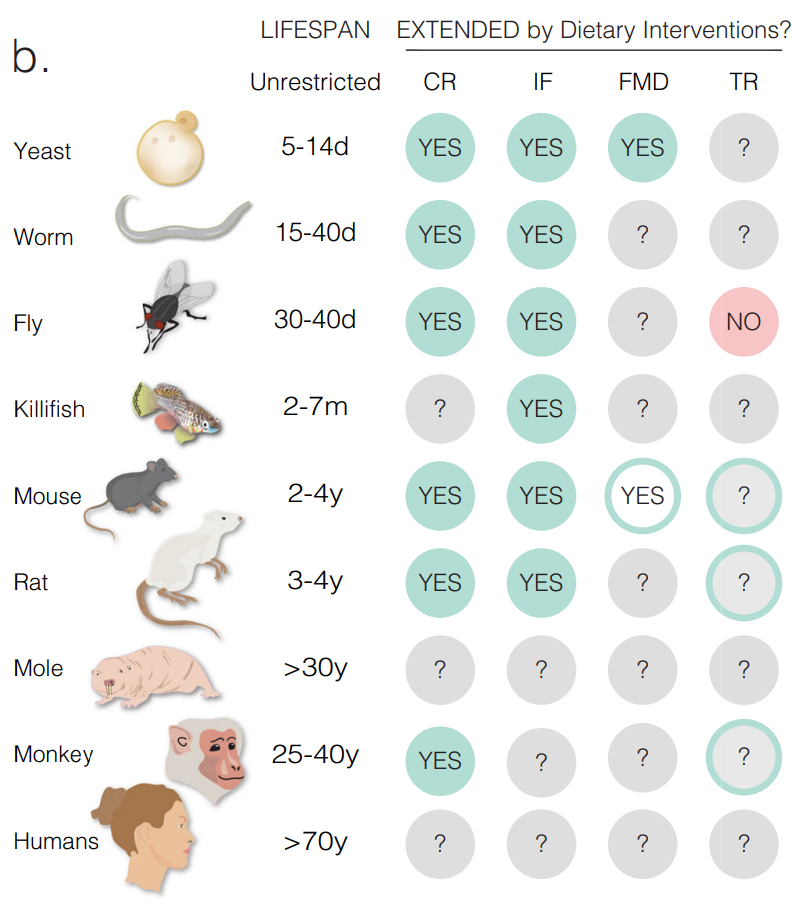
Option #1: Caloric restriction (in humans)

I made a whole blog about this, but in short there are not much human data. The NIH/NIA-sponsored 2-year CALERIE study demonstrated weight loss and greater insulin sensitivity, lower cardiovascular disease , and improved biomarkers of liver health. Further the pace of aging appears delayed using a “methylation clock” (Belsky et al., 2020). The similarities between the human, nonhuman primate, and mouse responses to CR argue for strong conservation in the underlying mechanisms by which CR impacts health in mammals, with links to improved longevity consistent between mice and monkeys but result may be dependent on weight loss.
Option #2: Time Resisted Eating in humans
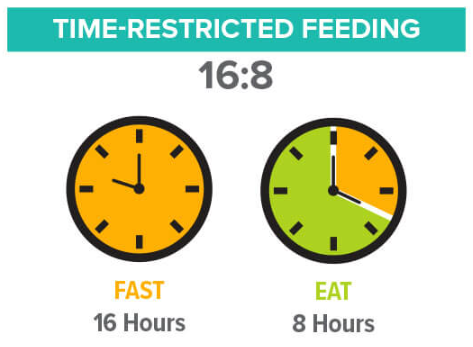
There is growing evidence of the beneficial effects of TRE also in humans (Duregon et al., 2021). Usually a 8–10 h daily eating window, with duration varying from 4 to 12 weeks. Almost all studies of TRE report weight loss and a reduction in adiposity or waist circumference when measured.
Several studies report improvements in circulating factors linked to cardiovascular disease, but this is not always the case. Epidemiology studies are less clear about TRE. Longer daily fasting periods that involve breakfast skipping have been consistently associated with increased mortality, which is particularly high for cardiovascular disease (Rong et al., 2019).
4 weeks of another form of intermittent fasting in which subjects fast every other day (alternate day fasting) was also effective in improving cardiovascular markers, reducing trunk fat, improving the fat-to-lean ratio, and increasing b-hydroxybutyrate, even on non-fasting days (Stekovic et al., 2020).
Option #3: Low-carbohydrate Diets

In humans, most low-carbohydrate diets limit daily carbohydrate consumption to 50–60 g, with the rest of the calories coming from high levels of fat and moderate to high levels of proteins. This sounds sensible but the evidence is not good.
Ketogenic and other low-carbohydrates diets have also been studied extensively in humans. In obese humans, a recent meta-analysis suggested that ketogenic/low carbohydrate consumption was no more effective than a balanced diet including low-calorie, low-fat/high-carb, or low-protein/high-carb diets, with equivalent effects on body mass index (BMI), circulating levels of total cholesterol, lipoprotein profiles, and triglycerides. Some large epidemiological studies have specifically focused on carbohydrate intake and mortality.
One of these studies followed 85,168 women (aged 34–59 years at baseline) and 44,548 men (aged 40–75 years at baseline) without heart disease, cancer, or diabetes, for 26 years and 20 years, respectively. This study showed that a low-carbohydrate diet based on animal food sources was associated with higher all-cause mortality in both men and women, whereas a low-carbohydrate diet with a higher content of plant-based food was associated with lower all-cause and cardiovascular disease mortality rates. Men on an animal products-based low-carb diet also displayed a 66% increased risk of cancer mortality, whereas women on the same diet displayed a 26% increased risk of dying of cancer (Fung et al., 2010).
In a meta-analysis of multiple cohorts involving 432,179 participants, both a low carbohydrate consumption (70% of energy) increased mortality risk compared to moderate carbohydrate intake. The risk of overall mortality increased by over 50% in the group consuming less than 20% of energy from carbohydrates compared to that for the group consuming 50%–55% of energy from carbohydrates (Seidelmann et al., 2018).
Notably, the low carbohydrate intake necessitates increases in protein and fat intake, raising the possibility that the higher protein and/or fat intake may be more important for mortality than the low carbohydrate consumption. In addition to macronutrient balance, the source of macronutrients was also found to be key. Mortality risk was about 18% higher when animal-derived proteins or fats replaced carbohydrates but 18% lower when plant-based proteins or fats replaced carbohydrates.
Option #4: High Protein Diets

The role of protein intake in increasing mortality is worrying. Whereas consumption of more than 20% of calories in the form of proteins is associated with a 75% increase in overall mortality risk and 400% increase in the risk of cancer mortality in subjects 65 years old or younger compared to consumption of less than 10% of calories from proteins, these associations are not observed in those 66 and older (Levine et al., 2014).
These results are in agreement with those in mice in which, prior to 85 weeks of age, mortality is minimized by a low protein consumption, but as animals aged beyond 85 weeks, a major increase in the protein to carbohydrate ratio is necessary to minimize mortality (Senior et al., 2019).
Option #5: Low Fat Diet
For decades, low-fat diets have been adopted by the public and recommended by the medical community to combat obesity. Although the consumption of fat has decreased in the United States, obesity has continued to increase pointing to increased total calorie intake and to modern diet composition rather than simply the intake of fat as culprits. In fact, when 7,447 participants at high risk for cardiovascular disease were randomized to a Mediterranean diet supplemented with extra-virgin olive oil, or mixed nuts, or to a control diet with the advice to reduce dietary fat, the risk of major cardiovascular events was about 30% lower in the Mediterranean diet groups supplemented with healthy fats from olive oil or nuts compared to the group recommended a low-fat diet (Estruch et al., 2018).
These results are also in agreement with the epidemiological data discussed earlier and showing that a diet high in animal fat and animal protein increases mortality compared to a high-carbohydrate diet, but that a low-carbohydrate diet is beneficial when high in vegetable-based food sources.
Option #6:Vegan Diet
Several studies indicate that pesco-vegetarians but not vegans display reduced risk for overall mortality compared to meat eaters, although a vegan dietary pattern is also associated with reduced risk of cancer, hypertension, and diabetes compared to that for regular meat eaters (Segovia-Siapco and Sabate´ , 2019).
However, the vegan diet has been associated with a 43% increased risk in all fractures and 2.3-fold increase in hip fractures compared to non-vegan diets (Tong et al., 2020). This frailty may be explained in part by deficiencies of certain amino acids. In fact in the EPIC-Oxford study, 16.5% of vegan men and 8.1% of vegan women had a protein intake lower than their requirement, which could be made worse by the reliance on amino acids solely from legumes, which provide very low levels of methionine and other amino acids.
In summary, the data are consistent with remarkable benefits of a vegan diet against aging and diseases but also an association of vegan diets with fewer benefits compared to vegetarian or pesco-vegetarian diets, possibly because these diets prevent the frailty associated with vegan diets in the general population.
Option #7:Combined Longevity diet
So far, there is no best diet, but combining all the best bits then we get a hint that the following combination of macros is least harmful:
65% carbs 20% fats 14% protein 1% spices/additives
A high(ish) carbohydrate with low (but sufficient) protein intake that is mostly plant based but includes regular consumption of pesco-vegetarian-derived proteins might be best (maybe with 12–13 h daily fasting period). This is similar to the classic “blue zones” geographic areas associated with human longevity:
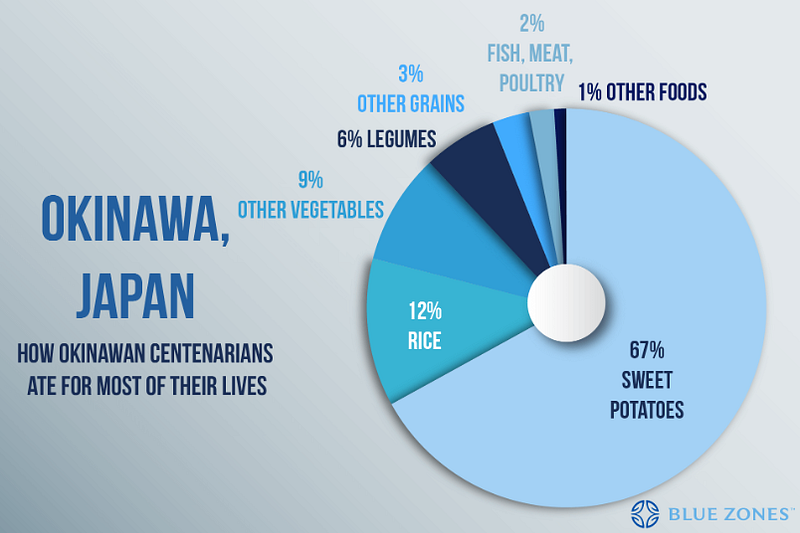
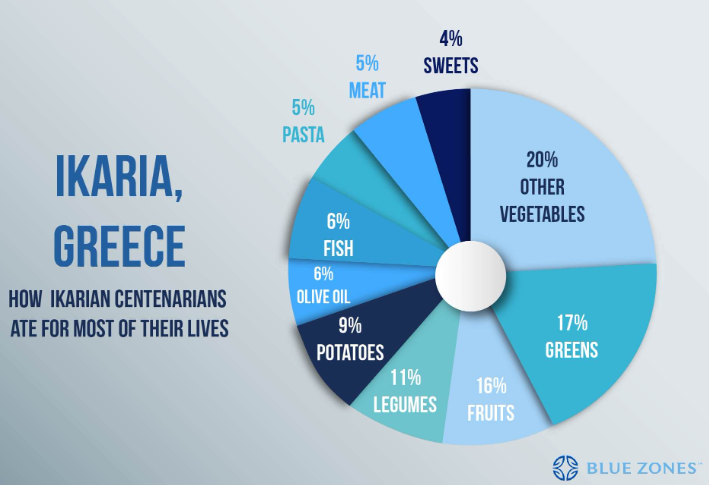
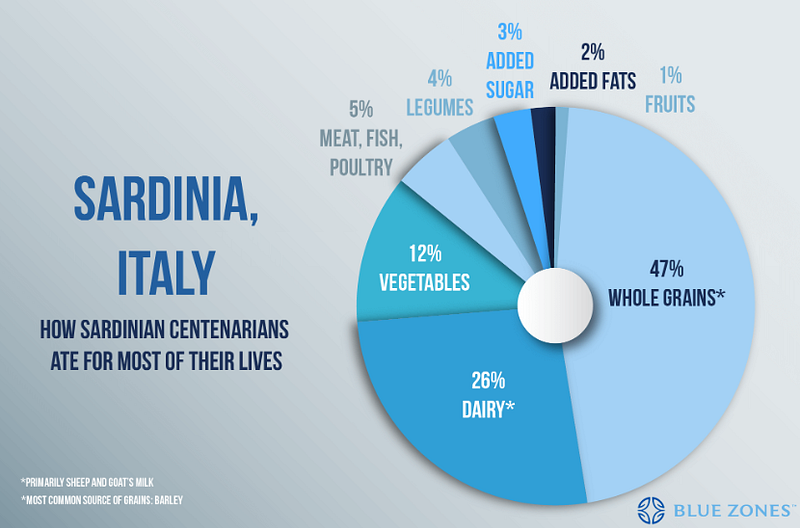
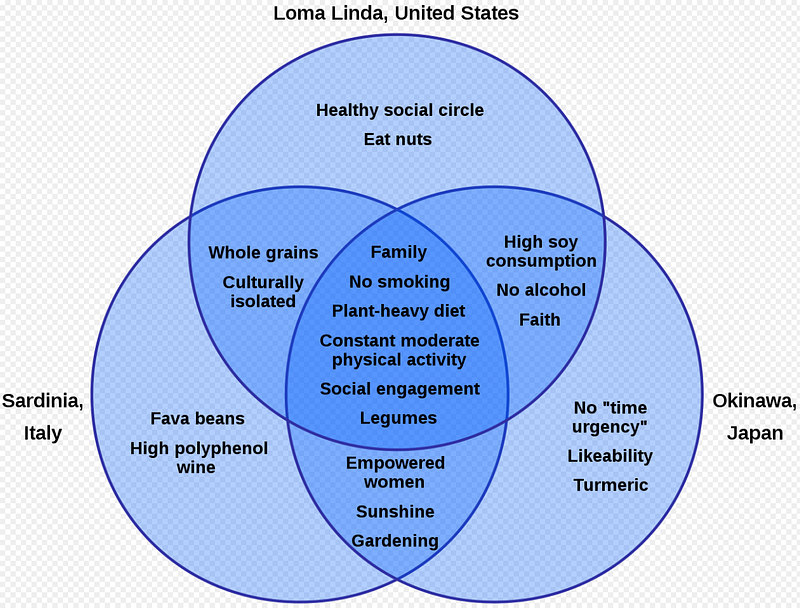
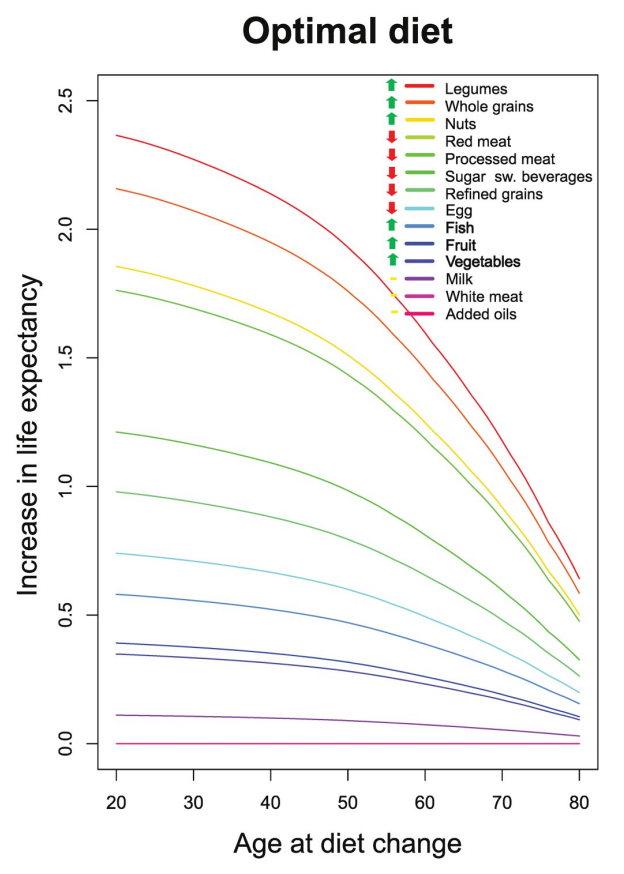
A recent study based on meta-analyses and data form the Global Burden of Disease 2019 study including studies from the United States, China, and Europe provides evidence in support of the longevity diet. A sustained change from the typical Western diet to an optimal diet rich in legumes, whole grains, and nuts with reduced red and processed meats is associated with an increase in life expectancy of 10.7 years in females and 13 years in males if started at age 20, and over 8 years of increased life expectancy when started at age 60 (Fadnes et al., 2022).

An important caveat is that the longevity diet should be designed to avoid malnourishment, particularly in the over-65 population, to prevent frailty and diseases that may result from reduced bone or muscle mass or low blood cell counts.
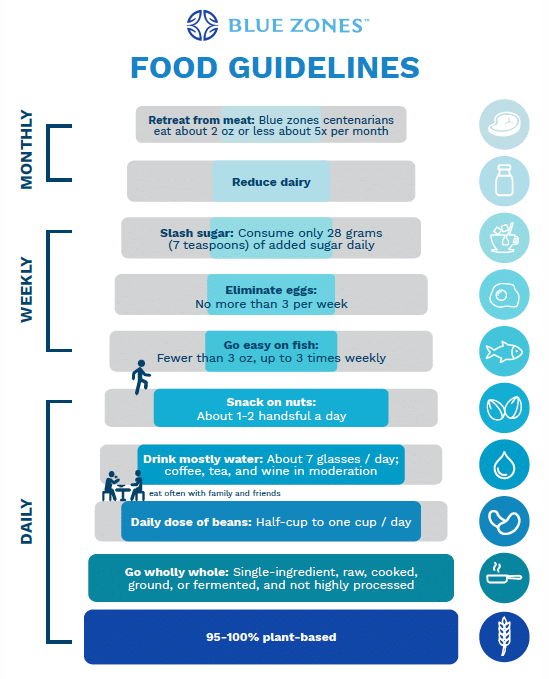
Take-Home Eating ADVICE
WHAT NEXT??
If you want us to assess your diet and its impact on your healthspan and lifespan we offer that here: https://shop.cyclingapps.net/biological-age-health-report/
If you want us to send you a meal plan including a healthy recipie everyday….we offer that here
CITATIONS
Belsky, D.W., Caspi, A., Arseneault, L., Baccarelli, A., Corcoran, D.L., Gao, X., Hannon, E., Harrington, H.L., Rasmussen, L.J., Houts, R., et al. (2020). Quantification of the pace of biological aging in humans through a blood test, the DunedinPoAm DNA methylation algorithm. Elife 9, e54870. https://doi.org/ 10.7554/elife.54870
Duregon, E., Pomatto-Watson, L.C.D.D., Bernier, M., Price, N.L., and de Cabo, R. (2021). Intermittent fasting: from calories to time restriction. Geroscience 43, 1083–1092. https://doi.org/10.1007/s11357-021-00335-z
Estruch, R., Ros, E., Salas-Salvado´ , J., Covas, M.-I., Corella, D., Aro´ s, F., Go´ mez-Gracia, E., Ruiz-Gutie´rrez, V., Fiol, M., Lapetra, J., Lamuela-Raventos, R.M., Serra-Majem, L., Pinto, X., Basora, J., Munoz, M.A., Sorli, J.V., Martinez, J.A., and Martinez-Gonzalez, M.A. (2018). Retraction and republication: primary prevention of cardiovascular disease with a mediterranean diet. N engl J med 2013;368:1279–90. N. Engl. J. Med. 2013, 368–1290. https://doi.org/ 10.1056/nejmc1806491.
Fadnes, L.T., Økland, J.-M., Haaland, Ø.A., and Johansson, K.A. (2022). Estimating impact of food choices on life expectancy: a modeling study. PLoS Med. 19, e1003889. https://doi.org/10.1371/journal.pmed.1003889
Fung, T.T., van Dam, R.M., Hankinson, S.E., Stampfer, M., Willett, W.C., and Hu, F.B. (2010). Low-carbohydrate diets and all-cause and cause-specific mortality: two cohort studies. Ann. Intern. Med. 153, 289–298. https://doi. org/10.7326/0003–4819–153–5–201009070–00003
Levine, M.E., Suarez, J.A., Brandhorst, S., Balasubramanian, P., Cheng, C.W., Madia, F., Fontana, L., Mirisola, M.G., Guevara-Aguirre, J., Wan, J., et al. (2014). Low protein intake is associated with a major reduction in IGF-1, cancer, and overall mortality in the 65 and younger but not older population. Cell Metab. 19, 407–417. https://doi.org/10.1016/j.cmet.2014.02.006.
Rong, S., Snetselaar, L.G., Xu, G., Sun, Y., Liu, B., Wallace, R.B., and Bao, W. (2019). Association of skipping breakfast with cardiovascular and all-cause mortality. J. Am. Coll. Cardiol. 73, 2025–2032. https://doi.org/10.1016/j.jacc. 2019.01.065
Seidelmann, S.B., Claggett, B., Cheng, S., Henglin, M., Shah, A., Steffen, L.M., Folsom, A.R., Rimm, E.B., Willett, W.C., and Solomon, S.D. (2018). Dietary carbohydrate intake and mortality: a prospective cohort study and meta-analysis. Lancet Public Health 3, e419–e428. https://doi.org/10.1016/s2468-2667(18) 30135-x.
Senior, A.M., Solon-Biet, S.M., Cogger, V.C., Le Couteur, D.G., Nakagawa, S., Raubenheimer, D., and Simpson, S.J. (2019). Dietary macronutrient content, age-specific mortality and lifespan. Proc. Biol. Sci. 286, 20190393. https:// doi.org/10.1098/rspb.2019.0393.
Segovia-Siapco, G., and Sabate´ , J. (2019). Health and sustainability outcomes of vegetarian dietary patterns: a revisit of the EPIC-Oxford and the Adventist Health Study-2 cohorts. Eur. J. Clin. Nutr. 72, 60–70. https://doi.org/10. 1038/s41430–018–0310-z.
Stekovic, S., Hofer, S.J., Tripolt, N., Aon, M.A., Royer, P., Pein, L., Stadler, J.T., Pendl, T., Prietl, B., Url, J., et al. (2020). Alternate day fasting improves physiological and molecular markers of aging in healthy, non-obese humans. Cell Metab. 31, 878–881. https://doi.org/10.1016/j.cmet.2020.02.011

